

Worker's Compensation Cost Reduction
Worker's Compensation Cost Reduction Captivated by the benefits of premium recovery?
A claims administration program will provide all the benefits of premium recovery without having to wait years to recover.
Human Resource & Administration services provide the opportunity to capitalize on technology, practicality & cost reduction. Specialized procedures for Workers Compensation, Fleet Management & Property & Casualty insurance.
Underwriters look for companies who operate lean and mean. Through implementation of an efficient HR and Insurance Administration, costs and hazards are controlled, leading to better rates across all policies and programs.
For over 2 decades National Risk Services has provided these services to Fortune 500, Small & Medium Business alike. You are a free consultation away from solving all your workers compensation problems.
Contact us today for your no cost, no obligation consultation with one of our Workers Comp professionals.
An In-Depth Look at Assisted Claims Handling
The following is a demonstration of the difference between an experience rating that reflects claims that were handled by an adjuster with only the First Report of Injury and no available resources and an experience rating that reflects claims that were handled by an adjuster who had both the First Report of Injury and all the available resources. It provides an in depth look at the drastic difference in experience modification factors and the actual handling of the claims themselves.

Description of Claims
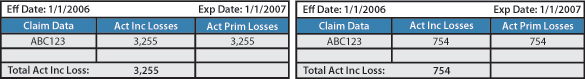
Claim #: ABC123
This is a scenario where an adjuster did not close the claim properly. At the time that the third report was set to be reported to the NCCI Rating Board, the Actual Incurred amount for this claim was reported as $3,255. If the adjuster had closed the claim at the proper time, it would have been reported to the rating board in the amount of $754.
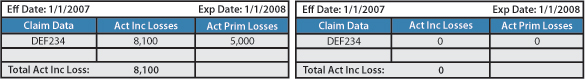
Claim #: DEF234
This is a scenario where an adjuster did not handle a dismissal case properly. This claim was dismissed due to lack of prosecution of the plaintiff. The adjuster did not decrease the reserve amounts to reflect the correct paid to date amount of $0. Instead, the adjuster let the claim sit on the experience rating at the original reserve amount of $8,100.
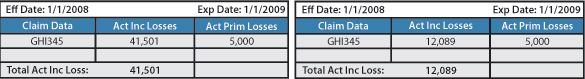
Claim #: GHI345
This is a scenario where an adjuster was not given the proper information to determine that this claims has a potential subrogation. This particular claimant was involved in a motor vehicle accident and sustained a broken leg. With the lack of proper paperwork and communication with the adjuster, they were only aware that the claimant sustained a broken leg. Therefore, the claim remained on the experience rating at the amount of $41,501 without pursuit of the deserved subrogation recovery. If the claim had been handled correctly from the beginning and the subrogation recovery had been obtained, the amount reported on the experience rating would have been reduced to $12,089.
Unexpected Benefits - From Government Regulation
Since WWII, many new programs, state and federal, regulating disability have been added to workers’compensation. In some states, short term disability is req uired for most businesses. All have to comply with OSHA and ADA. Social Security Disability Benefits claims involve many employers, directly and indirectly.
With the laws have come statutes, rules and regulations – at times overlapping other laws or even contradicting them. The wealth of material that must be read to deal with interactions is enormous – and well worth reading.
Many situations which are confounding if a solution is sought by staying within one law can be solved by searching the provisions of other laws. For example, obtaining an early independent medical examination shortly after an incident has been reported.
An independent medical examination under, say, New York compensation law must be done by the carrier in such a way as to comply with numerous requirements. Miss a single step and you must start over – which makes the first exam unlikely in less than three to six months. Some states restrict the number of independent exams on a claim, resulting in hoarding opportunities for an exam until late in a claim.
But other laws, free from the oversight of a comp board, often require exams for compliance. OSHA, in 29 CFR 1904.5, lists a variety of reported conditions that do not need to be listed on the OSHA Form 300. However, in order to comply, an independent medical exam would often be required, since only a medical professional, with access to prior records, could decide if an incident is one of the conditions subject to exclusion.
In such cases, an employee could be required to attend an exam and, in addition, provide HIPAA releases for prior records. And, the exams are not subject to local work comp laws or oversight. The report of the exam can be used in a comp claim if proper discovery procedures are followed – and the exam does not count as a work comp exam.
ADA can also be used for return to work examinations, again, with HIPAA releases. “Reasonable accommodation”, an ADA requirement, may often depend on the results of the exam. Again, the exam report can be used in the comp claim and the exam does not count as a comp IME.
Perhaps the most extreme example of expanding opportunities for additional exams is found in the New York Disability Benefits Law, WCL Sect 217(2), where an employer is given the right to have an employee receiving short-term disability benefits attend an examination once a week for the period of disability (for the maximum of 26 weeks of benefits). Short-term disability benefits are often paid while a comp claim is being contested. In such cases, a number of examinations could be scheduled and none would count as a comp IME.
These are but a few of the examples of how the myriads of laws already in force can, with some searching, provide new solutions to old problems. Searching outside the comp law is truly searching “out of the box”.
Theodore J. Ronca, Esq.
(631) 722-2100
Aquebogue, NY
12/30/10
Two Laws are Better Than One - for Work Comp Problems OSHA and ADA
For the employer, solving persistent problems in work comp is a matter, it is assumed, for the broker, the agent, the carrier or TPA, the WC Board or an attorney – but never the employer. In recent decades, the problems have grown more complicated, due to additional laws such as OSHA and ADA.
Few people in work comp, however, are asked to be sufficiently involved in OSHA or ADA to have deep insight into the possibilities of coordinated action. Literally nothing has been written on the subject, since it was assumed that such a subject did not exist.
It comes as a surprise, therefore, that two pressing problems in work comp can be solved by using two federal laws which, at first, seem to have little direct interaction with work comp. The first problem is obtaining an early IME exam following an injury, the second is proper structure of and incentives in a return to work program following extensive lost time.
A comp carrier, or TPA, finds it difficult to impossible to have an independent medical exam of an injured worker take place in less than four to six months from date of accident. The normal process of a comp claim does not automatically call for an early exam. Even if it does, Board rules and procedure, plus scheduling with a doctor, mean months of waiting.
However, if an employer could schedule an IME in the first week or so the entire course of the comp claim would be different.
Recently, attention was focused on a section of OSHA, 29 CFR 1904.5, which describes a wide variety of conditions which do not have to be reported on Form 300. But it requires a med exam, with prior med records, to decide if a reported condition is covered by the section. An employer, therefore, would be allowed to schedule a prompt exam and request HIPAA releases for prior medical records. Furthermore, a carrier or TPA would NOT be permitted to schedule such an exam, since they cannot act outside the comp law.
Similiarly, prior to a trial return to work, an employer may schedule, under ADA, an exam to see if accommodations are necessary. Again, HIPAA releases can be required.
In both cases, the exam records and results are not part of the comp record. And the costs are not added to the comp claim, or the experience modifier. However, with proper procedure and use of a subpoena, they may be released and used in the comp claim.
Why do such exams have a positive effect on comp claims? Why are they any different from an exam scheduled by a carrier or TPA? The answer lies in “employer involvement”. Most workers are surprised, and troubled, to discover that the employer has a much smaller role in comp than they imagine. A carrier, usually unknown until an accident, is, and remains, a remote stranger who speaks in incomprehensible terms and is never seen.
After a workplace accident, the first question asked of a worker by the spouse is, “What did the employer do for you?” If the answer is “Nothing.” morale plummets. If, on the other hand, the employer remains involved, even to the point of scheduling an exam, workers, and their families, are reassured. A worker, who is exaggerating, or falsifying, a report, also takes notice of such uncharacteristic concern by the employer and rethinks further efforts to overstate an injury.
OSHA and ADA are, however, just the tip of the iceberg in coordinating defense of claims. FMLA, short-term disability, SSDB and ERISA also have little explored features for defense.
The benefits, for the employer and employee, of imaginative coordination are impressive. Claims which formerly resulted in years of lost time can be limited to a few months. Unworthy claims can be substantially reduced - but only if the employer takes the trouble to be involved. This is one effort that cannot be delegated.
Theodore J. Ronca, Esq.
(631) 722-2100
Aquebogue, NY
2/7/11
| Today's Insurance News |
|
Updated 24 Hours a Day |
| National |

